The 5-Step Cervicogenic Headache Protocol
I can’t remember when I had my first headache, but it was sometime in my early 20s. I’ve had a lifetime of headaches. My headaches have been the bane of my life but also my constant companion and gift.
Last Saturday, en route to a barn dance, I had a whopper of a headache. I’m not too fond of perimenopause for the resurgence of headaches in the last two years. However, if it were not for my headaches, I would never have found Dr Brian Sher (Toronto Chiropractor), who provided my first neck adjustment that vanished my headache on the spot and paved the way to Chiropractic college. For that, I am immensely grateful.
Free Posture Crash Course!
Discover the crazy, simple 3-step formula that will teach you how to improve your posture and flexibility like a pro. You will learn how to hardwire the habit of good posture, reduce forward head and the secret way to stop slouching. It's 100% free!
Headaches changed the trajectory of my life, for the better.
Here’s the problem that I see with headaches. Most people burdened by headaches can not think clearly enough to take the steps necessary to rid their lives of the misery of chronic pain.
I get it – that was me!
I couldn’t get through the day without a muzzy painful head. I didn’t really know why I was having daily headaches, I just wanted to be like everyone else, who smiled and laughed and went to work and generally just got on with life.
That wasn’t me. I was working for the Sports Clubs of Canada at the time. I remember being at my desk, rubbing my head in misery while trying to complete my sales calls. The pain wasn’t particularly dramatic – it just seemed to be there more days than not. It was a burden, a drain, a constant weighing down. Life didn’t feel as good with a headache.
One day, I discovered I didn’t have to live my life with the burden of a headache. That was the moment I had my first Chiropractic adjustment, and that moment changed my life.
Recently, I’m reminded of what it is to have chronic headaches, due to my current hormonal haze of perimenopause. A resurgence of headaches has me eager to share my knowledge of headaches, and how I survive and treat my own headaches successfully – for the most part. I am quite certain this can help you too.
Cervicogenic Headaches
The term “cervicogenic headache” was actually coined in 1983. Although there is a long-standing notion that headaches can originate from structures in the neck and can be treated using manual approaches, it is only during the past two decades that the topic of cervicogenic headache has gained attention in the mainstream medical literature.
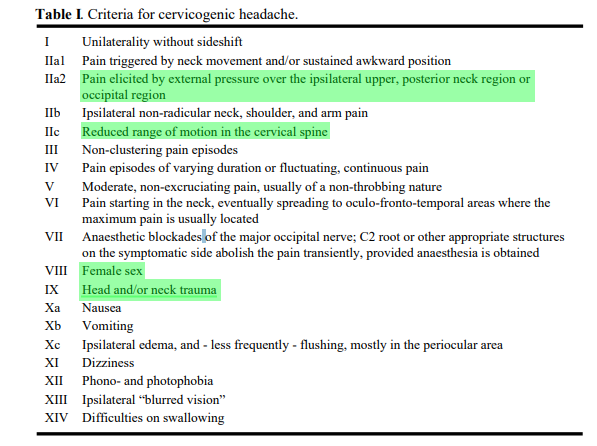
Signs and Symptoms
The cervicogenic headache is described as a unilateral or one-sided headache, generally starting in the neck and moving forwards. The headache generally dominates on one side. When the headache is severe, however, it may also be felt on the opposite side, but to a lesser extent.
There are also signs pertaining to the neck, such as reduced range of motion in the neck and mechanical stimulation applied on the affected neck area reproducing the headache symptoms. These strongly suggest cervical involvement in producing headaches. Sometimes, same-side shoulder/arm sensations and even pain have been reported.
People with a cervicogenic headache may report that the pain fluctuates, is continuous, lasts only a very short period of time, begins after long intervals, or starts up upon waking in the morning.
Prevalence
Studies support that cervicogenic headache is common. However, there is a great deal of variation in the perceived prevalence in the general population. For example, prevalence rates seem to range from 0.4% to 80%. It seems the disparity is due to contrasting diagnostic criteria being used in each study. The average affected age is 43,2, and the female/male distribution appears to have more agreement in the literature at 80% female, 20% male.

Cause
There appear to be three main causes of cervicogenic headaches discussed in the literature.
Convergence:
The basic premise of convergence is that when sensory nerves (first-order neurons) detect information about mechanical, thermal, and chemical states of the body and send signals back to the spinal cord, they converge on other nerves (second-order neurons) that carry signals from the spinal cord to the head. Pain signals from the periphery then get perceived as pain in the head and face, where the second-order neurons carry signals to the head (brain).1
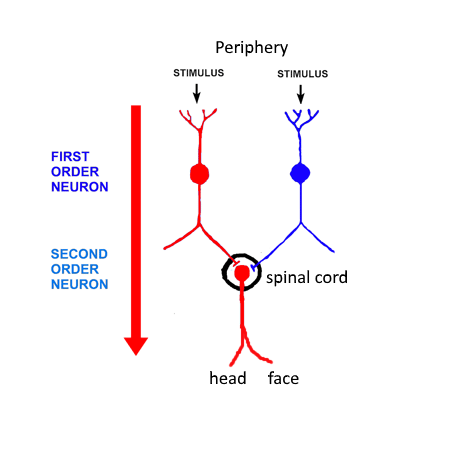
Degeneration:
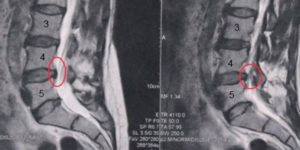
Disc degeneration, or degeneration in the neck’s facet joints, can cause inflammation and lead to irritation of sensory nerve endings for pain, called nociceptors.
Trauma:
In my clinical experience as a Chiropractor, trauma is frequently overlooked and a common cause of cervicogenic headache. If you have a history of trauma – in particular, a past motor vehicle accident – and a history of chronic headaches, you need a cervical x-ray series to rule out structural changes to your natural neck curve (lordosis). These changes (flat curve – alordosis, or reversed neck curve – kyphosis), lead to degeneration and altered mechanics in the neck, which cause inflammation and irritation of the nerve endings responsible for pain.
The prevalence of joint pain (facet joints in the neck) after whiplash from a car accident has been reported as high as 54%.3
Neck Disability Index
Before you begin my cervicogenic headache protocol, I recommend you measure your starting point regarding self-reported disability. Howard Vernon developed a tool called the Neck Disability Index (NDI) in 1989. The NDI has become one of the standard evaluations for measuring disability due to neck pain and is used by both healthcare professionals and researchers. There are just 10 questions, and answers for each are scored from 0 to 5. The maximum possible score is 50.
You can see a copy of my own NDI report. Note my moderately high frequency of headaches (a recent resurgence since peri-menopause).
Bookmark the link to the Neck Disability Index and complete the evaluation before you begin my headache protocol and every month along the way, to objectively measure your progress in terms of disability.
Cervicogenic Headache Protocol
I’ve created an entire online course to help you treat your own cervicogenic headaches effectively; and I’ve also extracted a mini version for you here, which consists of 5 steps:
- Neck Disability Index: Complete the NDI before you progress through this protocol.
- Neck X-Rays: Have a cervical series of x-rays taken through your doctor or directly from your Chiropractor. Many Chiropractors have their own on-site digital facility, as I did. The standard series is Cervical AP (front to back) and Cervical Lateral (side view) and often APOM (an open mouth view to visualize the first two vertebrae C1 and C2). If in doubt as to why you need a neck x-ray to proceed, please refer back to the section Cause above and review the third cause, trauma.
- Range of Motion: Review the section above on signs and symptoms of cervicogenic headache. Reduced range of motion is almost always present in the neck of someone with cervicogenic headaches. Whether or not the lost movement is the cause or the effect isn’t clear, but I stand by the need for increasing your cervical range of motion.
- Trigger Points: Myo-fascial trigger points, also known as muscle knots, are painful spots in the fascia (connective tissue) surrounding the muscle. Trigger points in the neck and shoulders are commonly associated with referred pain in the head. Refer back to the signs and symptoms above. Recall that manual pressure applied to the affected neck area producing headache strongly suggests cervical involvement. So although self-applied trigger point therapy might initially bring on a headache (please use with caution); the idea is that regular administration, will lead to a reduced frequency and/or severity of cervicogenic headache.
- Stretch: After range of motion exercises and trigger point work, it is crucial you stretch your neck to elongate the muscles out to their full length. Although stretching as a treatment is going out of style, I still find it immensely beneficial, and stretching often reduces or eliminates my headache on the spot!
It probably works about the same way that stretching out a calf cramp works: you win the tug-of-war with the spasming muscle. Paul Ingraham
If you enroll in my How to Get Rid of Headache and Migraine, I know it will help you. In the course, you find out everything I know about headaches and learn the actual exercises and techniques I’ve used so successfully to treat my own chronic headache pain for over two decades. These exercises have the potential to alleviate even the most chronic of headaches. Not only do I cover my top seven self-treatment techniques, but I also teach you how to rule out worrying red flags, give you several ergonomic best practices and share with you the top three researched methods for outsourcing headache treatment.
If you don’t enroll, the Cervicogenic Headache Protocol above will be an excellent place to begin.
Resources:




One thought on “Cervicogenic Headache Exercises”
I am fascinated by your videos and would like to use part of the video called “FORWARD HEAD POSTURE CORRECTION” for my lectures I present through PESI HEALTHCARE and some independent seminars on FALL RISK; FALL PREVENTION and NEUROLOGICAL CONSIDERATIONS in FALL RISK. This last topic is a lecture i will be presenting at the REHAB SUMMIT in LAS VEGAS NEVADA in NOVEMBER. I will address POSTURE and postural changes with aging and how this impacts on fall risk in older adults. I would give you FULL ACKNOWLEDGMENT by name and by your website if this meets with your approval. I look forward to your reply ! Your material is excellent and will reach clinicians that could use this knowledge immensely ! THANKS FOR YOUR TIME !